After an aunt and a friend in her 30s were diagnosed with breast cancer, Beth Kunkel made breast self-examinations part of her daily routine in the shower.
During one of those checks in October 2017, Kunkel, at age 37, felt a slight change to a benign spot on her left breast that she’d been paying attention to for about six years. She had it checked by Dr. Ellen Hopper, her Sanford Health obstetrician and gynecologist, which led to a mammogram, an ultrasound, a biopsy by general surgeon Dr. Kelly Ming and ultimately a diagnosis: HER2-positive invasive ductal carcinoma breast cancer.
Kunkel caught it relatively early, in stage 2, but it’s one of the most aggressive types of cancers that’s prone to recurrence. Rather than have a lumpectomy with radiation, she opted for the more drastic alternative: double mastectomy with immediate breast reconstruction and chemotherapy.
Her reasoning: She was young, had two children, now 8 and 10, and was done adding to the family, and would have a much smaller chance of getting breast cancer.
“Peace of mind. And I know my personality would always be thinking, ‘I felt another lump,'” she said.
Nipples and skin saved
Some mastectomies involve removing the entire breast and then stretching or expanding the skin over time to eventually allow for breast reconstruction. Kunkel’s plan involved one surgery with two steps and a minor procedure later.
First, Sanford Health breast surgeon Dr. Jesse Dirksen in Sioux Falls, South Dakota, removed all the breast tissue through incisions in the fold under each breast, similar to the scar location for breast augmentation. Tests on that tissue also revealed precancerous cells in her (opposite) right breast — more confirmation she made the right decision to get a mastectomy.
Then plastic surgeon Dr. Heather Karu, also with Sanford Health, inserted implants above the muscle in each breast pocket, which allowed Kunkel to keep all of her skin and both nipples. That is generally possible unless a tumor location prevents it.
“I went to sleep with breast cancer and woke up with new breasts and no cancer,” Kunkel said.
She did lose all sensitivity in her breasts but anticipated more of an emotional adjustment to the loss of feeling. The relief of being cancer free and now less prone to future cancer more than made up for it.
Three months after the surgery, Dr. Karu took fatty tissue from Kunkel’s abdomen and inserted it around each breast implant as a cushion to give it more of a natural look and feel.
Less pain, recuperation
Dr. Karu was among the first doctors in the region to start performing pre-pectoral breast reconstruction three years ago in which the implant is placed above the muscle. Personally, as a woman who has breast cancer in her family, and as a physician, she also would choose it if she were diagnosed.
“That makes it easy for me to offer to my patients. I don’t have any hesitation about what a nice result I can provide for them,” Dr. Karu said. “Most of our patients go home after one day. It’s decreased patients’ pain, and women are usually pleased with how they look aesthetically. The shaping you can achieve in one stage is wonderful.”
That’s because it takes advantage of the skin already there for the breasts, instead of stretching the skin or taking it from another part of the body, she said.
Breast reconstruction doesn’t entirely eliminate the chance of breast cancer, since about 2-5 percent of breast tissue remains, but it significantly decreases the chances, Dr. Karu said. “Everyone has to keep doing self exams. That continues to be an important part of monitoring lifelong.”
Different bra size
After a breast cancer diagnosis, most of the focus is on treating the disease — the “rain cloud” of cancer, Dr. Karu said. By the time she talks to the patient, the discussion about mastectomy and breast reconstruction actually can be a “silver lining” of sorts because the woman can change her appearance as part of the treatment.
“Although cancer is an awful way to get there, sometimes the cancer allows them to have the equivalent of an augmentation, a reduction or a lift at the time,” Dr. Karu said. “I always start by asking, ‘What size are you now and would you like to be the same size, bigger or smaller.’ A lot of the As want to be bigger, Bs and Cs the same size and some Ds smaller or perkier. Their goals are my goals.”
Most patients are pleased by what they see the next day when the bandage comes off and they look in the mirror for the first time, Dr. Karu said.
“Wow, this looks good. I didn’t expect this at all,” Karu said, regarding the usual reaction. “To get that response is such a home run.”
Breast reconstruction is actually required by a law Congress passed 20 years ago called the Women’s Health and Cancer Rights Act of 1998. It requires insurance companies to cover the cost of not just treating the cancerous breast but reconstruction on both breasts, if that gives the woman a symmetrical look, Dr. Karu said.
Chemo and cool caps
Kunkel, from Watertown, South Dakota, said she caught her cancer early largely because she knew what was normal and what wasn’t. She needed the added tests because younger women have denser breast tissue that can make it difficult to spot a cancerous tumor. Once her doctor confirmed the spot was suspicious, her medical insurance covered the cost of the mammogram and all other procedures.
After the nipple-sparing mastectomy and breast reconstruction, she underwent weekly chemotherapy treatments for seven hours over 12 weeks, then 90-minute treatments every three weeks, which she will complete on Oct. 30, one day shy of her first treatment.
Kunkel, an optometrist, practices with her husband and father, so she has had the flexibility to make those appointments, which involve 200-mile round trips to Sioux Falls.
Besides the surgery, the other obstacle to fighting cancer with chemotherapy is the loss of hair. For Kunkel, this was a big deal because she loves having her kids brush her hair and didn’t want to lose that comfort at a time when she needed it most. Her son offered to make her a stocking made out of yarn, so he and his sister could continue that special time, if Kunkel did lose her hair.
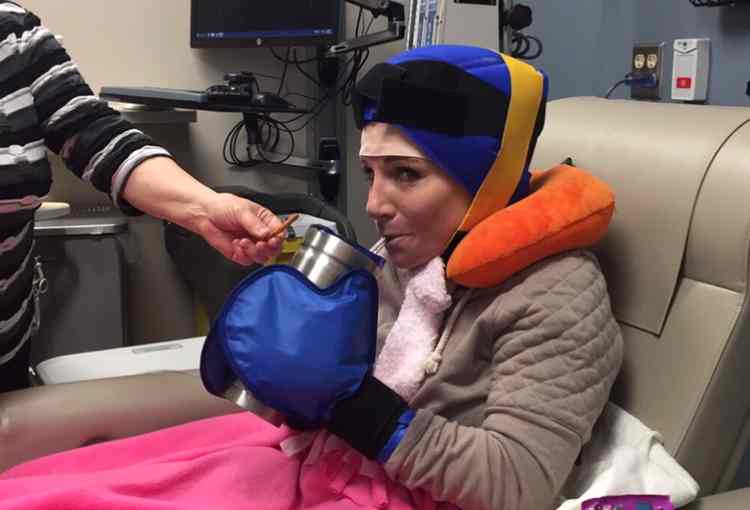
But because of cool cap therapy, she was able to keep her brown, shoulder-length hair. The treatment entailed her wearing a gel cap on her head to cool the scalp during chemotherapy.
“It was the thing that my kids were most concerned about and scared about, so I wanted to shield that from them,” Kunkel said. “But for me, I wanted to go out grocery shopping and out to eat and not have people look at me like I was sick or treat me differently.”
Helping other breast cancer survivors
As she nears the end of her chemo treatments, Kunkel finds herself helping a lot of other women who are themselves shocked by the diagnosis and seeking answers to treatments — some good to come from her bad.
“On my Facebook page I put that it was a year since my double mastectomy. People were commenting, and five or six were my new friends I met this year through breast cancer,” she said. “It’s people I’ve never met. Through telling my story on Facebook and CaringBridge, someone has heard of it and they get ahold of me. And I just tell them what they have in store and how it was for me. It’s just that emotional support.
“When you get diagnosed, out of the woodwork you quickly gain this support group of other people going through it.”
…
Posted In Cancer, Cancer Screenings, Cancer Treatments, Imaging, Watertown, Women's