Sanford Health, the largest rural health system in the country, launched the PLEDGE Study to identify and predict which children may be at risk of developing type 1 diabetes (T1D) and celiac disease.
The Leona M. and Harry B. Helmsley Charitable Trust awarded Sanford Research with a grant of $1.3 million for this study, which will conduct screenings for infants and children during routine visits at all Sanford Health locations in Sioux Falls, South Dakota, and Fargo, North Dakota.
This is the first time a population screening for T1D will be offered in the Midwest.
Learn more and enroll: PLEDGE pediatric screening study
“A recent trial has shown that we may be able to delay the onset of type 1 diabetes — if we can identify who has already started down that path,” said Dr. Kurt Griffin, a pediatric endocrinologist at Sanford Health. “Type 1 Diabetes TrialNet has been a successful screening program for autoantibodies with relatives who have type 1 diabetes, but this excludes 90% of the children who will go on to get diabetes.
“The Sanford PLEDGE study allows us to offer this screening more broadly, integrated into routine care to minimize any burden on families or providers.”
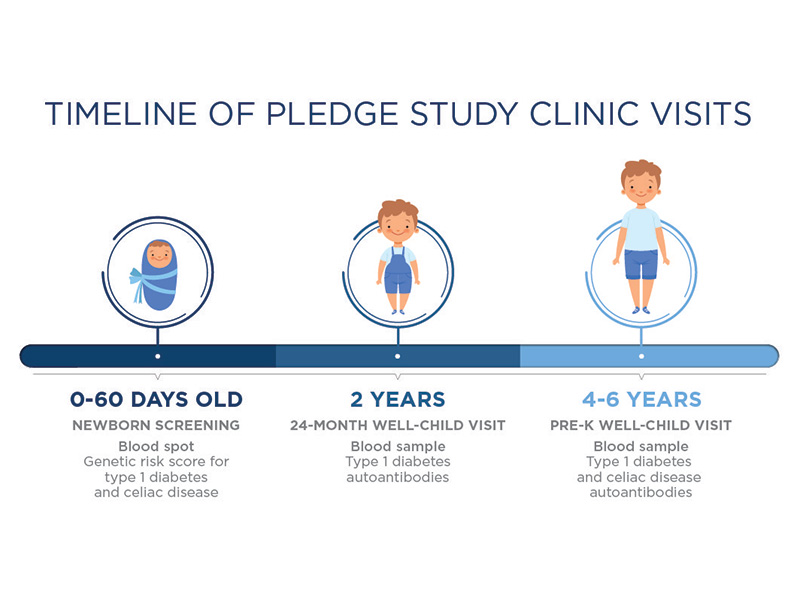
Graphic by Sanford Health
How PLEDGE works
Depending on a child’s age when entering the study, a small amount of blood will be collected while being seen for routine care around birth, 2 and 5 years old.
For children found to have autoantibodies related to T1D, Sanford Health providers will be able to offer education, monitoring and early intervention to prevent serious illness at the time of diagnosis and to improve long-term outcomes.
When appropriate, Sanford will also offer participation in T1D prevention clinical trials to delay or stop the progression of T1D.
“We are committed to improving the lives of people impacted by T1D, including those at risk of developing the disease,” said Anne Koralova, Ph.D., Type 1 Diabetes Program Officer at the Helmsley Charitable Trust. “Increasing screening can have a major impact on the health of these at-risk individuals. We’re excited to partner with Sanford Health on this innovative initiative.”
Autoimmune diseases’ impact on kids
1 in 200 people in the U.S. have T1D. T1D is an autoimmune disease that destroys the beta cells that make insulin. Over time, this causes high blood sugar levels, which left untreated are life-threatening.
Currently, lifelong treatment with insulin for those with T1D is required to control the blood sugar levels and maintain health. For many children, T1D develops unexpectedly and may take months or years to progress from the start of autoimmunity to having high blood glucose. Ninety percent of T1D diagnoses occur without a family history.
The lifelong autoimmune disease, celiac disease, develops unexpectedly and often with no symptoms right away. Left untreated, serious damage to the small intestine and other organs can occur. Children found to have autoantibodies related to celiac disease will be referred to clinical care for further evaluation.
Why sign up: Meet a family enrolled in the PLEDGE Study
While traditional clinical trials require clinical coordinators to enroll patients, the PLEDGE Study will allow parents to consent electronically through their My Sanford Chart accounts, and have labs drawn during routine pediatric care, which should encourage greater participation.
“Now is the time when we can justify expanding type 1 diabetes autoantibody screening,” said Dr. Griffin. “What we learn from the Sanford PLEDGE study will help develop the evidence needed to add this screening to standards of care.”
Parents can enroll their children in the study if they are 5 years of age or younger, receiving routine care at Sanford Health and not diagnosed with T1D. An annual questionnaire will be sent to parents until the child’s seventh birthday to update their medical history.
To learn more or to enroll in PLEDGE, talk with your child’s primary care physician or visit sanfordhealth.org.
Learn more
- Artificial intelligence helps spot diabetes risk
- Crohn’s, ulcerative colitis patients reclaim lives with help
- Newborn screenings: Why do them? What’s the benefit?
…
Posted In Children's, Digestive Health, Endocrinology, Research
