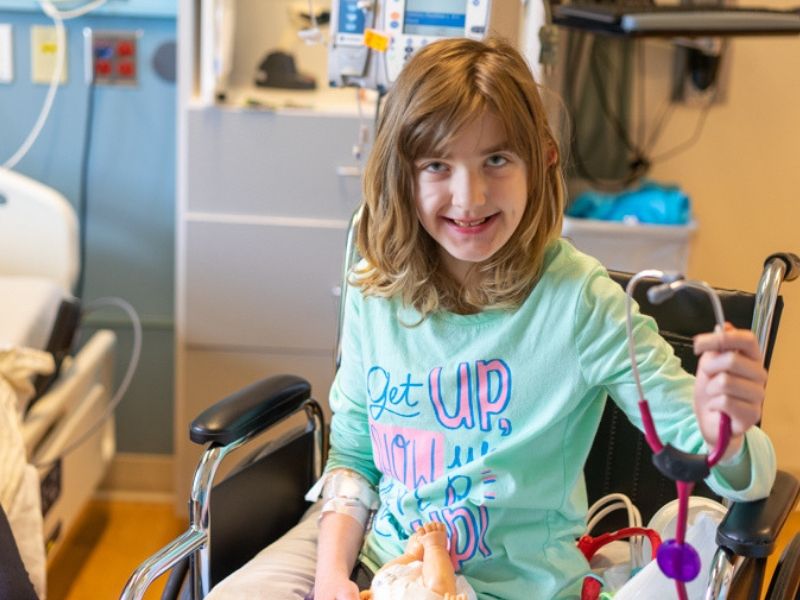When you meet Kaley Maassen, you first might be struck by the 11-year-old’s beautiful shoulder-length hair. Besides looking shiny and smooth, the curls at the bottom appear too perfectly shaped to be natural.
If you’re used to looking at a daughter whose hair sticks out in every direction within 10 minutes of brushing it, Kaley’s hair seems like a dream.
Kaley’s life, however, has been a lot more tangled. A lot less smooth. Not an effortless dream, but thanks to her good nature, her family and medical support, also not an impossible nightmare.
Before birth, ultrasounds gave parents Joel and Brooke Maassen a hint that their second child might have an abnormality. An MRI shortly after Kaley’s birth at Sanford USD Medical Center in Sioux Falls, South Dakota, confirmed that she had a small brain with excess fluid.
Soon after that, the newborn’s then-unknown condition led to spinal and rectal surgeries — the beginning of more than 50 surgeries she’s tallied at Sanford Health so far.
Within a couple of months of Kaley’s birth, her parents found out the rare diagnosis for her. With the help of Sanford Health pediatric genetics specialist Laura Davis-Keppen, M.D., they learned Kaley lacked an end segment of a chromosome.
“When the chromosome 6 diagnosis came back, that helped give us some more answers,” Brooke said. “She’s the only one in South Dakota with it, so it’s a pretty rare chromosome condition.”
Enlarge
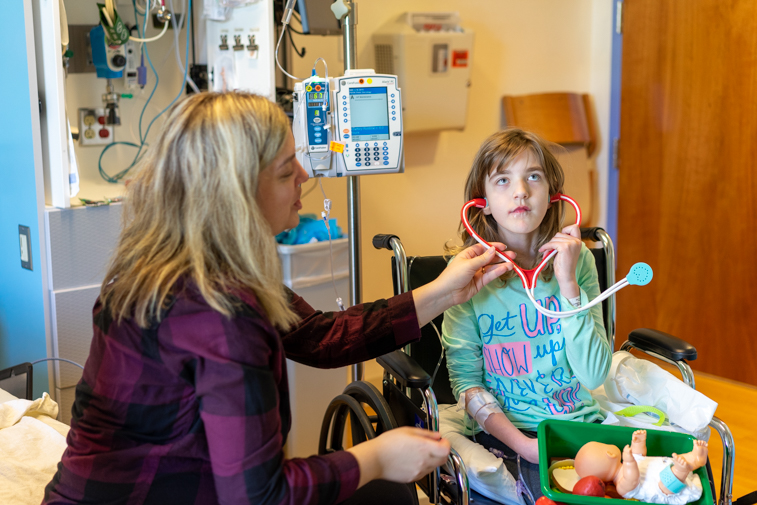
Kaley’s particular chromosome disorder is so uncommon it’s difficult even for her doctors to find much information about it. But she has a whole team behind her who have become familiar with the challenges it has caused. Those range from developmental delays — she didn’t walk till she was 3½, for example — to feeding difficulties and dental issues. She experiences delays in school as well.
Adding to team of children’s specialists
By the time Kaley reached age 9, the medical team included her primary care doctor and a Sanford Children’s pediatric neurologist, gastroenterologist and surgeon.
Then, a mystery illness put Kaley in Sanford Children’s Hospital in Sioux Falls, with symptoms including nausea, vomiting, fatigue and a fever up to 107 degrees. The cause was elusive — until another kind of specialist got involved. The kind of specialist a parent prays to never have to see.
With Kaley’s nonspecific symptoms, a PET scan and bone marrow test were used to determine that, on top of her other health issues, she had large B-cell lymphoma, too, involving her neck area, bones and bone marrow.
“Hearing the cancer diagnosis for her was very scary,” Brooke said.
Kaley’s family turned to a Sanford Children’s pediatric oncologist for treatment, expertise and guidance. They found continual support from him, along with the nurses, child life specialists and staff teacher they worked with during Kaley’s treatments.
She had to stay in Sanford Children’s Hospital for four days every other week for five months while receiving chemo treatments.
“Basically everybody knows her because she was here so much,” Brooke said.
Brooke and Joel were grateful Kaley could be treated so close to their Brandon, South Dakota, home, at South Dakota’s only pediatric oncology unit. It allowed them to switch off staying at the hospital (also known as the Castle of Care) or going home at night with Kaley’s brothers.
“What’s nice about the Castle is they do have enough specialists here now that you don’t have to go to another state. Because going to another state when you have four children and a child that’s so sick, you just want to be home. You want to be close to home. You don’t want to have to travel if you can help it,” Brooke said.
Comparable care here
Kaley’s pediatric oncologist, George Maher, spends his days treating children with cancers ranging from leukemia and brain tumors to lymphoma and kidney tumors. Even outside of South Dakota, patients may get referred to the Sanford Children’s oncology unit in Sioux Falls from southwestern Minnesota, northwestern Iowa and as far as Wyoming.
Enlarge

Dr. Maher may work with the University of Minnesota or Mayo Clinic to coordinate care for certain procedures or expertise not offered at Sanford Children’s Hospital, such as stem cell transplants or proton beam radiation. But otherwise, he said, the doctors here stay in contact and collaborate on cases with oncologists across the country about the best treatments for cancers and, as a result, can provide care comparable to larger institutions.
In addition to the more common pediatric cancers such as leukemia and brain tumors, “we are constantly encountering things that are rare in children or rare generally that we just have to kind of review and educate ourselves,” Dr. Maher said.
“If it’s something that I’m not sure of, I’ll call the national expert. … Pediatric oncology is kind of a close‑knit society. The person you’re calling knows what you’re up against.”
And for treatments, Dr. Maher said, “we’re all singing off the same sheet. We’re all using the same up‑front chemotherapy regimen.”
That’s an assurance for families. “That’s why we’re here — so that the patients don’t have to drive four hours to Rochester,” he said. And to keep an arduous time in a family’s life from becoming even more difficult.
Getting to know families
Brock Doubledee, a Sanford Children’s pediatric gastroenterologist, treats problems in children ranging from reflux and constipation to inflammatory bowel disease. He has seen Kaley and her family regularly since she was an infant having feeding difficulties, including gagging and retching problems.
Enlarge

She had a gastrostomy tube (G-tube, or feeding tube) placed early. She has significant sensory issues, such as texture, and doesn’t like eating very much. So she still gets 90% of her nutrition through the feeding tube, Brooke said, to be sure she continues to gain an appropriate amount of weight.
Because of her sensitivities and complications of her chromosome disorder, Dr. Doubledee doesn’t expect her feeding issues to change a lot. And those kinds of cases are the hardest part of his job, he said: “At times, patients like Kaley, you can’t always effect the change you want to. You can’t just simply make them better.”
But he, along with the other children’s specialists, still has seen improvement with Kaley. Dr. Doubledee said developing a relationship with families is rewarding. “I think getting to know them on a somewhat personal level helps you to take care of them better because you understand, to some degree, the family dynamic and everything else that’s going on.”
Kaley doesn’t seem to mind her continual trips to see the children’s specialists.
“When we go to the doctor now, every time we go, she asks for paper and a clipboard, and then she asks us questions,” Brooke said.
“You know you’ve been at the doctor a lot when your favorite thing to do is play doctor.”
Hospital stays
Kaley is not fond of entering the hospital, however — something she had to do recently to try to identify and treat an infection. Typically, her stay starts out with getting an IV tube inserted, which she hates.
Brooke said it doesn’t work as well for her to be in the room, since Kaley wants her mom to “save” her from it, so she entrusts Kaley to a child life specialist, whose job is to help children cope with a hospital stay through methods such as playing. Kaley routinely asks for an iPad, and the child life specialist plays games on it with her. The child life specialists supply her with toys, activities and attention throughout her stay as well.
“They take such good care of her, and I just feel like they treat them like their own children,” Brooke said.
Enlarge

This hospital stay brought back memories for the whole family of Kaley’s cancer, since she was experiencing similar symptoms. “It was pretty nerve-wracking for us this week — just not knowing,” Brooke said. “Because it was exactly two years ago to the day that she started showing symptoms of the cancer. It was really hard for us, thinking is she having a relapse, or is this something else?”
As it turned out, it was an infection that invaded Kaley’s body. This is due to her lowered immunity because of her bout with cancer. Not long before this, she had had whooping cough, and pneumonia had preceded that.
The lows and highs
Relapse is understandably on the mind of parents who have watched their children struggle through cancer treatments. It’s also something Dr. Maher dreads.
“Their lives are back together, and they come in for a routine visit, and the nurse says that Pathology is on the phone. And you know immediately what that means. They saw something,” Dr. Maher said. “And then you have to drop that bombshell on the family. They all know it’s possible, but … it’s heartbreaking.”
On the other hand, one of the best parts of treating children with cancer, he said, is when they finish their chemotherapy treatments. At Sanford Children’s, they get to ring a bell and have a celebration that includes staff, too.
“It is something to celebrate,” Dr. Maher said. “You get them through a very, very rough bit of therapy, and they should be proud of themselves.”
Teaching program for longer-term patients
Sanford Children’s Hospital is the only hospital in South Dakota with a teaching program for children, according to Barb Acheson, who retired recently as the hospital’s schoolteacher.
The teaching position at the hospital coordinates class assignments with the home school district of children such as Kaley, who end up hospitalized for longer periods of time. This helps students, when they’re feeling well enough, to keep up with their classmates. It also provides them with a diversion.
Kaley worked with Acheson during chemo treatments.
Enlarge

“The days get pretty long here, so it was nice just to have her come in and work on a few things, and her to do some worksheets,” Brooke said.
The teacher may coordinate work for up to 35 students at a time. If kids feel well enough, they can work at the center table in the Castle “classroom” on the third floor. Books and games abound here, and computers are available. Or the teacher or volunteers can help guide kids through work in their hospital room.
The benefits stretch beyond keeping busy or keeping up with classmates.
“When a child is here in the hospital, they’re probably at one of the most vulnerable times in their lives,” Acheson said.
Schoolwork gives them a piece of normal life back, and they want to do it, she said. “This gives them control at a point in their lives when they have no control.”
Acheson found her work meaningful. “You give a little piece of yourself to each and every patient,” she said.
In return, she added, “I have received more from my patients than I’ve ever given them.”
Brooke appreciated Acheson’s attentiveness. “She was always popping in here to see what she could do, or if she felt up to doing work today,” she said.
Positive attitude and gratitude
Kaley’s enviable hair is new since her chemo treatments. “She didn’t have curls before,” Brooke said. It came back a lighter color as well.
Kaley hasn’t had a haircut since then. You could say the length of her hair symbolizes the time she’s been free of her hardest health battle.
You could also say the beauty of her hair symbolizes the beautiful spirit she carries throughout her life, undimmed by all of her challenges.
Kaley always has a smile on her face, her mom said.
“Kaley very rarely complains. As sick as this child is so often, she will hardly tell you. We almost have to ask her,” Brooke said. “You can tell by her symptoms, but she very rarely tells you.”
Occasional bouts of frustration may arise because of her disorder and a younger brother — understandable to anyone who has had a younger brother — but “her attitude is very positive about life in general.”
Perhaps part of that could be attributed to her parents, who Dr. Maher said “do an incredible job with her.”
“Brooke and Joel have been amazing to work with. Not demanding, just appreciative,” he said.
“They’ll take whatever you have that can help them — very dedicated to Kaley.”
Brooke’s gratitude emerges as she reflects on Kaley’s experiences with Sanford Children’s and its specialists.
“It’s been a tough road, but we’re thankful for caring and loving people and a great hospital. It makes all the difference in our days when people help you get through it and tell you how much they care,” she said.
“It helps us feel like we can get through this bump in the road … and hopefully move on to better days.”
More stories
- Children’s specialty care: A team approach
- Genetic testing for pediatric cancer
- Diagnosing, managing a child’s developmental disabilities
…
Posted In Brain & Spine, Cancer, Children's, Digestive Health, Genetics, Inclusion at Sanford, Sioux Falls, Specialty Care