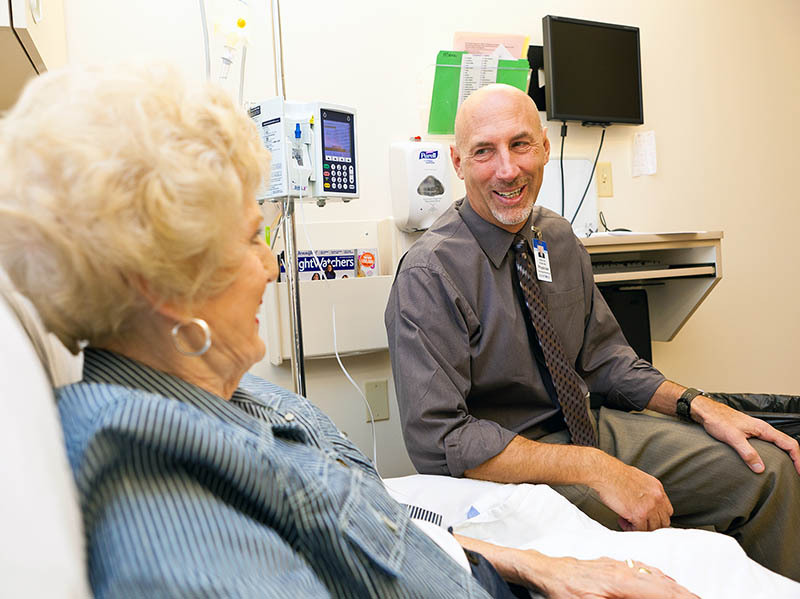
A diagnosis of cancer typically doesn’t end there. Next, a patient and doctor usually discuss a treatment plan that might involve surgery, chemotherapy, radiation or immunotherapy.
But how do doctors know how much chemotherapy a person with a certain type of cancer should have? The guidance they go by has its roots in clinical trials.
People who agree to participate in a clinical trial, and receive something possibly different than the standard care at the time, benefit many patients who come after them. Those patients will know they’re receiving the best quality of care.
Sanford Health makes participation in a variety of clinical trials a priority, said Tamara Fischer, a clinical research manager at Sanford.
“It’s a mission of Sanford to support research,” she said.
Fischer has a background as a chemotherapy nurse along with helping coordinate research trials. She currently serves as the administrator of a six-year federal grant Sanford Health received for patients to participate in nationwide cancer clinical trials.
Find clinical trials: Sanford Health studies enrolling near you
Preston Steen, M.D., a medical oncologist, is the principal investigator for the NCORP grant, which stands for NCI (National Cancer Institute) Community Oncology Research Program. The grant was approved in 2019 and will vary in funding from year to year, depending on how many patients participate. The other roughly half of Sanford Health’s cost to conduct the NCORP clinical trials is covered by the health system.
Sanford typically has about 60 adult NCORP clinical trials in progress, Dr. Steen said. Last year, Fischer estimates around 1,000 patients were enrolled. Sanford Research also conducts many other clinical trials outside of the NCORP umbrella.
Offering access
“Our main goal with the NCORP is to be able to provide access to either drugs that aren’t commercially available, or trying to determine what’s the best possible treatment,” Dr. Steen said. “Some of it might be drugs that are available but using them in a new way, or comparing what was previously the gold standard to something that looks like it might be better, so that people can have access to those things without having to travel to the Twin Cities or Mayo or further.”
Sanford Health is one of 46 NCORP groups, or “community sites,” across the U.S. enrolling patients into NCI-approved cancer clinical trials and research studies. Most of the clinical trial projects come from a regional research base.
If successful, the results of the clinical trials can make a big difference in cancer treatment, prevention and other aspects of care. They study a variety of cancers affecting the breasts, colon, lung, skin, brain and blood.
Developing new standards
Fischer recalls starting a clinical trial about two decades ago looking at a new drug for breast cancer. Herceptin was given to breast cancer patients who were HER2 positive, or positive for a protein that can encourage growth of cancer cells. The clinical trial was stopped early, Fischer said, because Herceptin was showing so much success in reducing recurrence rates of cancer.

Photo by Sanford Health
“So that is now a standard therapy that patients, anybody who is HER2 positive, will receive,” Fischer said. “So we have seen some big changes over the years due to the trials that we have done.”
As a more recent example, Dr. Steen points to a national chemotherapy clinical trial that Sanford Health patients with stage 3 colon cancer were enrolled in. The standard treatment at the time called for 12 cycles of chemotherapy two weeks apart — lasting about six months. But one drug, when taken that long, has a potential side effect of nerve injury. So the study compared outcomes for patients who had chemotherapy for six months vs. three months and discovered no difference for that subset of stage 3 colon cancers, Dr. Steen said.
“If you go back further to when I started,” he added, “people got slightly different drugs, but people with stage 3 colon cancer got a whole year of chemotherapy.” Clinical trials then had reduced that to six months.
Some trials may focus less on medications, side effects and prevention and more on cancer’s broader implications in patients’ lives. They might explore, for example, financial issues related to treatment.
Working together
Fischer and Dr. Steen have plenty of experience overseeing clinical trials. Fischer, who is based in Bismarck, North Dakota, has helped there for more than 30 years. The first NCORP grant Sanford Health received started in 2014 and lasted for five years. Similar programs preceded the NCORP program. Both Dr. Steen, based in Fargo, North Dakota, for about 30 years, and Fischer worked with the similar programs before the first NCORP grant.
The two of them meet regularly with Sanford Research managers in Fargo and Sioux Falls, South Dakota. They also talk with providers throughout the Sanford Health enterprise about new clinical trials coming out to decide whether they would be a good fit at Sanford Health.
While Fischer and Dr. Steen naturally contact oncology providers about clinical trials, they look to a variety of other providers to help identify eligible patients as well.
For example, specialists outside of oncology can let their patients know about screening trials. One such clinical trial opening soon, looking at benign pancreas cysts that could become malignant, will rely on gastroenterology specialists, Dr. Steen said.
And a large ongoing National Cancer Institute trial aims to enroll 165,000 women to examine the difference between 2D and 3D mammography. This randomized TMIST trial is open now to Sanford Health patients. The trial will try to determine definitively whether 3D is better than 2D mammography at detecting breast cancer.
Importance for patients
Generally, though, as medicine becomes more personalized, the drawback for clinical trials is that fewer patients are eligible as criteria have become much more specific, Fischer and Dr. Steen said. The trials may look at a specific gene mutation found in a much smaller population. And smaller studies may fill up with enrollees pretty quickly.
“So we have to be more innovative and more creative in terms of how we look at trials or patient populations,” Dr. Steen said.
Nevertheless, Sanford Health patients play an important role in these national trials. Involving more rural patients and more Native American patients improves representation for the overall study. In addition, it gives those patients greater access to cutting-edge, potentially life-saving research.
Fischer appreciates the changes she has seen in patient care in the past few decades. She has watched as many medications once considered experimental became the standard, or then were replaced by something better.
“Lung cancer, many years ago, was basically a death sentence. If you could make 18 months to two years, that was really a great thing,” Fischer said. “And now we’re seeing new treatments, and patients are living three to five years.”
Some multiple myeloma patients, she added, are getting 10 or 15 years compared to three in the mid-1980s.
New treatments, new outcomes — all made possible by clinical trials.
Read more
- Physician doing clinical trials in smaller, rural setting
- Network expands access to Minnesota cancer clinical trials
- How a clinical trial helps bring the latest in care to you
…
Posted In Bismarck, Cancer, Cancer Screenings, Cancer Treatments, Digestive Health, Fargo, Imaging, Research, Rural Health, Sioux Falls, Specialty Care, Thought Leadership