Until recently, it took a lot to get Ken Santema to see a doctor.
Even when he started having breathing problems, he waited as they worsened. Finally last summer, when walking just 20 feet would wind him and force him to sit down, he went to Sanford Aberdeen, South Dakota, to get checked out.
Santema first went through a couple of lung function tests. Then he asked the doctor if it mattered that he had a lump on his neck, which seemed like a bug bite.
The doctor immediately ordered a CT scan, which did not show a problem with Santema’s chest.
Instead, the CT scan revealed an enlarged lymph node pushing against Santema’s trachea and reducing air flow.
A biopsy explained the reason for the enlarged lymph node. It also pushed Santema into a lifelong journey he’d rather not be traveling: living with cancer.
Learn more: Cancer care at Sanford Health
‘Fireworks show’ of cancer
Santema has follicular lymphoma. That’s a form of non-Hodgkin’s lymphoma, or cancer of the blood. This particular form grows slowly, and treatment can send it into remission, but it’s difficult to cure.
Santema calls the day he had a PET scan, spotlighting the cancer cells in his body, “the fireworks show.”
“From head to thigh, I was lit up. My bones were all lit up with cancer. My spleen was huge and lit up with cancer. One of my lungs, a big portion of it was lit up with cancer,” Santema said. That didn’t count all of the bright lymph nodes all along the scan.
Some patients with follicular lymphoma have no symptoms and can delay treatment because of the cancer’s slow-growing nature.
Santema was not one of those patients. His case had advanced so much, and he had such a hard time breathing, that his Sanford Health oncologist recommended he start chemotherapy right away. He agreed. “I wanted to breathe,” Santema said.
Santema also wanted to live — not just for himself, but for his wife, Mindy, and their three sons, two in their teens and the other, age 22. He wanted to continue enjoying their idyllic, if small, home on a lake less than 20 minutes from Aberdeen, with its surroundings “right out of a Bob Ross painting.”

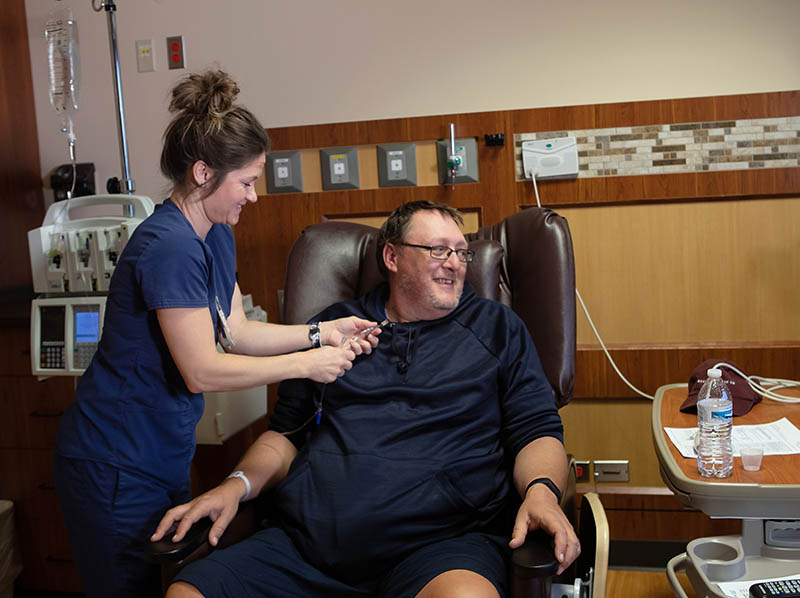
Photo by Lisa Johansen Aust, Sanford Health
The half-dose of Benadryl he received with each one make the chemo infusions themselves difficult to remember. However, he does recall that after his second day of chemo, he was outside working in their garden. “All of a sudden, I’m like, ‘Wait a minute. I’m walking around.’ I was breathing. I didn’t have to sit down after walking 10 steps.”
His hand went to his neck, and he discovered he couldn’t feel that lymph node anymore.
As cancer got better, chemo got worse
After his first round of chemo, a steroid had given Santema energy, and he could breathe again. Sure, he had side effects like trouble sleeping, lethargy and a metallic taste in his mouth, but “I remember thinking at the time, that wasn’t so bad.”
Also at this time, he started a new project to publicly document his battle with cancer. An experienced blogger about technology, project management and politics, he shifted focus when he started “Dad Against Cancer,” a blog about fighting lymphoma. In it, he writes about various aspects of cancer, including his medical and emotional experience, as well as his family’s experience.
After Santema’s third round of chemo, he had good news to report: A PET scan showed far less cancer, especially in his bones.
“It seems like after that is when the rounds of chemo got harder and harder,” Santema said. The cancer was fading, but the Army veteran “felt like I had been through war.”
Related: Ways to help recover from chemo
His sixth and final round of chemo came the day after Christmas. “I would’ve rather gone back on deployment again than go through another round of chemo,” he said.
Fortunately, Santema’s PET scan then showed him clear of the follicular lymphoma — a huge relief. “In the back of my head, there was always a nagging thought like I’m going to die soon,” he said.
He thinks he and his wife both cried that day, though he blames his tears on the prednisone steroid. He typically hasn’t cried as an adult, but now he might start crying over the death of a robot in one of those “cheesy sci-fi movies,” he said.
Strong support team
Santema now receives a maintenance infusion of rituximab, a monoclonal antibody that helps the immune system destroy cancer cells, every eight weeks for two years.
This infusion has unpleasant side effects, too. For days, “I feel almost but not quite like I have the flu,” he said. He also develops a cough that slowly improves over the rest of the eight weeks, then starts over again.
In light of this, Santema has been asked, “Why do you do it?”
He admits he thought about deciding against it. But “there is a chance that maintenance can extend the amount of time I’m in remission,” he said. He copes now because he hopes for a long future, even though it includes follicular lymphoma.
Learn more: Cognitive effects of cancer better understood
In the line of people Santema credits with helping him through his medical journey, his wife tops the list. Constantly by his side, “she’s been there asking the questions I don’t think of when we go to doctors’ appointments,” he said. At home, he loves gardening and canning with her for hours on end.
His sons, too, “stepped up so much,” Santema said. They did household chores their dad typically would have done, and they conscientiously sanitized and limited their dad’s exposure to germs because of his weakened immunity.
Santema calls out his Sanford Health care team, too. Dr. Jason Spjut, the surgeon who installed Santema’s chemo port, cracked jokes before the procedure.
“To me,” Santema said, “anyone that does surgery should be funny.”
And then there are the nurses. “They don’t make me feel like I’m their patient. They make me feel like I’m their friend,” he said. He’s impressed by all they remember about him and his family each time they see him.
Sources of peace
Santema has changed since his diagnosis — and not just in being more agreeable about seeing a doctor.
When he first learned he had follicular lymphoma, he immediately thought about death. His best advice now: “Breathe. … Don’t think death. Just think positive.” His cancer can’t be cured, but it can go into remission, and he can live a full life. And tomorrow may bring more advances for the fight.
Relaxing together can soothe the bad days. Sitting on the deck, watching the lake, listening to some country music: “There’s just nothing better in the world,” Santema said.
And his blog is not just an exercise in stress relief for himself, although writing out his stress does help. It also intends to help other people know that they’re not alone. And family members of cancer patients really respond to that by asking him questions and inspiring future blog posts.
“These family members, they’re just as much going through cancer as we are.”
…
Posted In Aberdeen, Cancer, Cancer Treatments, Imaging, Pathology, Pulmonology