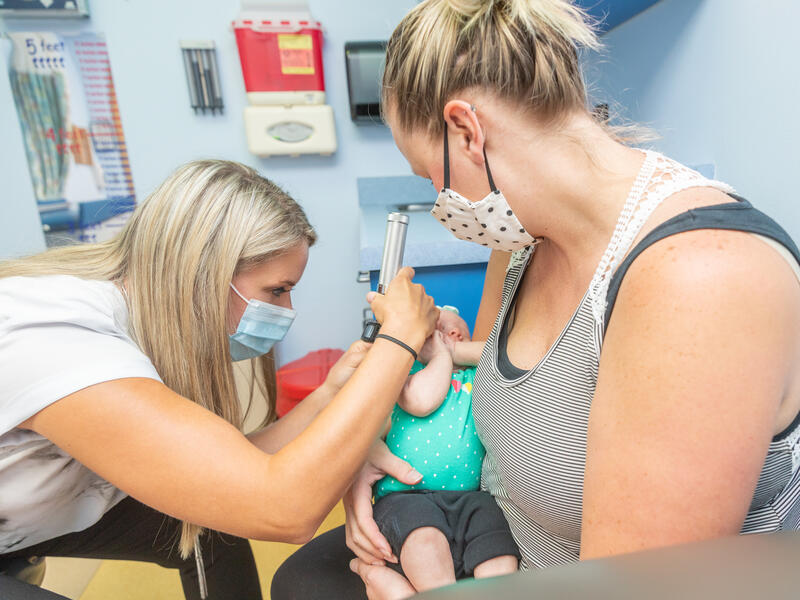
If advanced practice providers, or APPs, ever went away, you’d notice. They’re an irreplaceable part of health care.
Their reach goes far and wide. They work with physicians to see, and treat, patients of all ages.
Some patients have questions about APPs, and what exactly they do.
We’ve got answers.
Who is an APP?
Many providers fall under the umbrella term of an APP. They include:
- Nurse practitioners (NP)
- Certified nurse midwives (CNM)
- Certified registered clinical nurse specialists (CNS)
- Certified registered nurse anesthetist (CRNA)
- Physician assistants (PA)
- Audiologists
- Genetic Counselors
APPs provide multiple services for patients including:
- Diagnosing and treating conditions and illnesses
- Diagnostic tests, including laboratory and medical imaging
- Prescribing medications and alternate treatments
- Informing patients on health conditions and prevention of illnesses
- Communicating with physicians, nurses, social workers, pharmacists to ensure quality patient outcomes
What education do APPs have?
Ashley Lipp is a PA at Sanford Health in Clear Lake, South Dakota. She said PAs are APPs who have a master’s degree and are licensed to provide medical care with the supervision of a physician.
“We go through a full bachelor’s program in undergrad. Then, the school after that is onto a PA program. The one I went to at USD (University of South Dakota) is a full year of classroom learning. A lot of those classes are with the medical students. So, the PA schooling is very much in line with the medical school training for that first year,” she said.
After that comes clinicals.
“40, 60, 80-hour weeks of being strictly in the clinics. Every six weeks you go to a different location and different specialty. We have a little bit of knowledge in every field of medicine. We go from family practice to surgery, to cardiology or dermatology, (and) pediatrics,” she explained.
PAs have a different educational path than the rest of APPs. To become an NP, CNM, CRNA, or CNS, a provider must become a registered nurse first before continuing their education.
Nurse practitioners, for example, “have a bachelor’s degree in nursing; they’ve become nurses and have done a four-year college program for nursing. Then, they have gone on to the graduate level and received whatever specialization they work in,” explained Karissa Getting, CNP, from Sanford Health in Sheldon, Iowa.
“There’s a couple different branches, like midwives, nurse anesthetists, clinical nurse specialists, and they have very specific training for their area,” Getting added.
Where are APPs needed most?
APPs, in all forms, are critical. Especially in rural health care, “where there’s a shortage of physicians,” Lipp said.
“It is pretty special to find any providers that want to be in rural settings. I think that’s where APPs have really stepped up. When you choose to be in a rural setting, you chose it. That’s where you want to live and raise your family,” she added.
Find an APP near you: Search sanfordhealth.org/doctors
This helps to forge connections and relationships with patients who call rural America home.
“You’re living in the same community. You know the resources that your patients have and don’t have. It makes the patient-provider relationship even more special.
APPs are a big asset to rural communities and help keep care close to home.
Getting said APPs “have ongoing dialogue with physicians in larger cities,” as well as smaller cities in the area. If they have a question about how to help a patient, they can consult a physician.
“Otherwise, patients are having to drive an hour to a larger city, where there’s more medical providers to give them care. I do think we provide kind of a gap closure, if you will, for that. We’re sort of an extension of the medical doctors.”
Can an APP be my primary care provider?
Yes, they can be a primary care provider.
“I tell patients I’m going to provide the safest, best care. I reassure them that they will get the appropriate care. We have the training to do this, but of course, if a patient is still uncomfortable, we tell them we’ll talk with a doctor. It’s whatever makes them most comfortable. We do have collaborating physicians,” Getting explained.
Lipp said a patient can count on APPs to provide them quality primary care, “because we see everything and anything.”
“We do things from wellness physicals to child physicals when people are feeling well. We see people when they’re sick in acute care. We’ll cover anything from coughs and colds to abdominal pains or any acute issues.
“We take care of people as they get into their later stages of life for their chronic medical conditions. So, diabetes, hypertension, anxiety, depression, we will see patients for all of those things.”
Learn more
- When should I find a primary care provider?
- Vietnam War created PA training for rural, Native care
- Sanford announces $300 million for rural health care access
…
Posted In Children's, Clear Lake, Family Medicine, Here for all. Here for good., Internal Medicine, Physicians and APPs, Rural Health, Thought Leadership