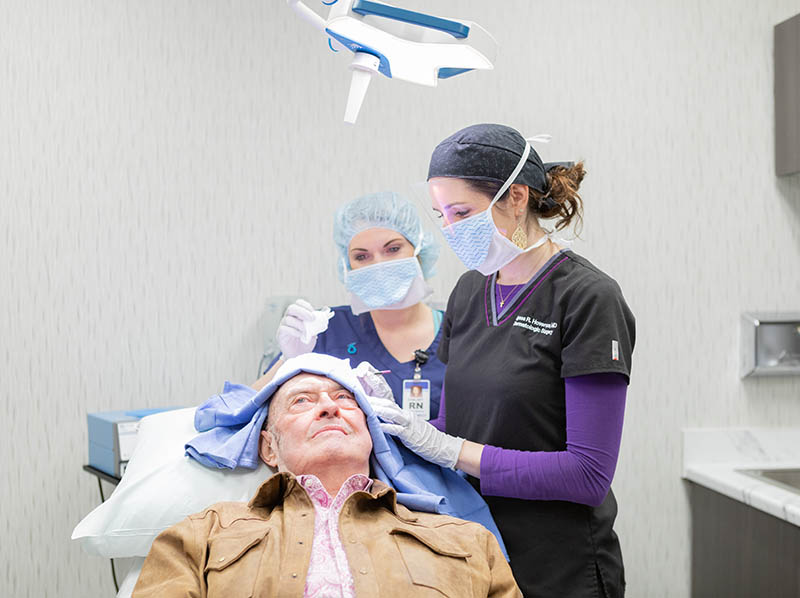
You could safely say Gary Burton has experience with Mohs surgery. He’s been through the skin cancer treatment at least 15 times.
You could also safely say he and his Sanford Health providers have gotten to know each other pretty well.
So well, in fact, that Burton’s surgeon, dermatologist Alyssa Hoverson, calls him “one of our favorite patients.”
So well that Burton jokes with them: “You guys are such nice people. I really wish you were at a profession where somebody actually wanted to come and see you.”
But Burton willingly travels 75 miles from his Lancaster home, in extreme northwest Minnesota, to Sanford Health’s dermatology clinic in East Grand Forks, Minnesota, to visit them regularly.
Burton, 78, has been plagued with new skin cancer spots for about four years, ever since a spot on his hand turned out to be skin cancer.
Surgery for skin cancer can involve excision, or cutting out the cancerous area and surrounding healthy skin. For the head and neck, though, Mohs micrographic surgery is the preferred treatment for the two most common skin cancers, basal cell and squamous cell.
Burton’s skin cancer “just kind of spreads itself around,” he said. He’s had it on his face, scalp, earlobe, neck, arms — and three times on his lip, one of the most painful spots.
Steps in Mohs surgery
Mohs surgery is the preferred treatment for the most cosmetically sensitive areas for a couple of reasons. No. 1, it has the highest cure rate — 99% — of any skin cancer surgery, said Dr. Hoverson, who received training during her residency at Mayo Clinic, and since then, to do Mohs surgery. And No. 2, it reduces the size of the scar.
Enlarge
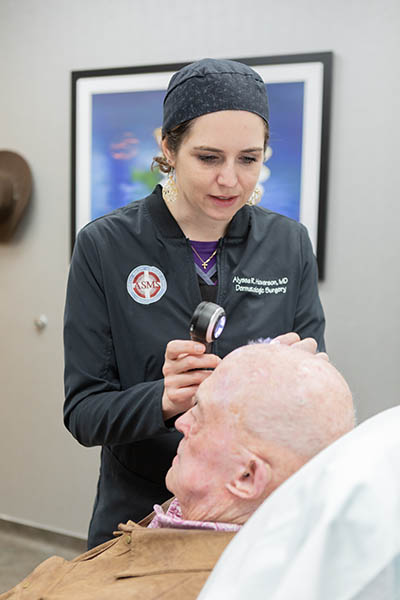
A three-step process helps accomplish these two goals.
The first step involves Dr. Hoverson doing surgery in the clinic to remove the entire tumor and a very narrow portion, or margin, of healthy tissue. That leaves intact as much healthy tissue as possible. Taking the first layer means, she explained, “we go around the cancer and a little bit deeper.”
The second step shifts Dr. Hoverson into the lab while the patient waits. With a microscope, she examines the edges of the tissue removed to be sure that part is clear of cancer. If she finds cancer cells in that margin, then she returns to the patient to remove more skin from just that particular, small area. Then she examines the new part under the microscope to be sure its margin is clear.
When Dr. Hoverson is satisfied she has removed every bit of the skin cancer, the third step involves closing the wound. How she closes the wound can depend on its location and its complexity. It may simply need stitches, or she may use a skin flap from an adjacent area, or she may use a skin graft from elsewhere on the body.
Find: A dermatologist in your area
Dr. Hoverson enjoys doing surgery and estimates that she performs about 34 a week. Mohs surgeries make up 24 of those.
The third Mohs step, along the lines of plastic surgery to keep the scar as minimal as possible, is Dr. Hoverson’s favorite part. “It’s like trying to figure out how to put everything back together and making it look nice,” she said.
Mohs surgery ‘a breeze’
Burton said once he gets past the few seconds when the shot of lidocaine is delivered to numb the area, “the rest of it’s a breeze.”
The Mohs surgery “goes amazingly well,” he said. “I’m not particularly in love with it, but it seems like it takes care of the problem.”
It can be a long day, depending on how many times tissue must be removed, so Dr. Hoverson tells patients to plan for a whole day just in case.
But after that, the patient typically needs no further treatment — just bandage care at home, then a follow-up appointment for suture removal.
Preventing need for Mohs surgery
Dr. Hoverson considers it important to educate her patients in addition to treating them. She talks with them about why they might have developed skin cancer. Some had significant sun exposure in the past, possibly from where they lived or their occupation. And she goes through preventive measures.
“We definitely recommend not using tanning beds,” she said. And going on vacation somewhere warm is great, she said; just be sure to wear sunscreen. She recommends SPF 30 or higher and reminds people to reapply it every two hours. Sunglasses and wide-brim hats help, as does UPF clothing.
While Burton was growing up in northwest Missouri, he rode a tractor with no cab and no shirt, he said. Now, he wears a cowboy hat all the time and applies a lot of sunscreen, hoping to slow down his skin cancer. Several times a year, he also undergoes photodynamic therapy, which uses a combination of a topical drug and a certain light wavelength to kill precancerous cells.
Burton urges others to be vigilant about their skin. “You get a dry spot or something don’t look right, then go somewhere and have it looked at.”
For her part, although she would prefer her patients’ skin to be healthy and require no doctor visit, Dr. Hoverson does love working with them, especially Burton with his positive attitude.
“When you’re doing surgery on them and they’re awake all day,” she said, “you really get to know them — hear their stories.”
More stories
- Melanoma survivor who had cancer at age 15: Save your skin
- Tanning bed dangers and safer alternatives
…
Posted In Cancer, Cancer Treatments, Dermatology, Grand Forks, Healthy Living, Plastic Surgery, Rural Health, Specialty Care, Thought Leadership