A sunny summer afternoon seems perfect for soaking up the rays. But that’s not where you’ll find Megan McManus. She sits in the shade, sharing an important message: Prevent cancer by protecting your skin.
“It’s easy to be convincing when you’ve had personal experience,” says the cancer survivor.
Skin cancer at 15
McManus figured the small growth on the left side of her face was nothing more than a long-lasting pimple. A doctor’s appointment and tests led to a devastating diagnosis: melanoma — the least common, most dangerous type of skin cancer.
At 15, she faced a tough course of treatment including multiple surgeries and chemotherapy.
“I was scared at first, then realized this is a bump in the road and I’ll get through it,” she says. “I also kept reminding myself that my doctors didn’t tell me I had months to live. Rather they told me I had months of treatment. There’s a big difference.”
In addition to her medical care with Sanford Health, McManus credits her faith, family and a wide circle of support for helping her through.
“Even my dad’s college buddies sent messages of encouragement,” she says.
About skin cancers

Skin cancer is the uncontrolled growth of skin cells that leads to the formation of tumors. This can happen anywhere in your body, but it is most common on sun-exposed areas. Skin cancers are generally classified as either melanoma or nonmelanoma skin cancers.
Nonmelanoma skin cancers can often appear as large pimples that bleed, red warts that scab, pink freckles, or a bump that hurts and does not go away. You also might not even notice them. They rarely spread to other organs, and they can be treated with surgery.
Melanoma, in most cases, is either an old mole that changes, or a new mole that appears. These always look different from normal moles. People with red hair, blue eyes and pale skin have a higher risk for melanoma, but it can happen to anybody.
“In general, the lifetime risk of skin cancer is about one in five,” says Alyssa Hoverson, M.D., a dermatologist at the Sanford Dermatology Clinic in East Grand Forks, Minnesota. “Specifically for melanoma, it’s one in 38. Overall, a very significant amount of people are going to be affected by some kind of skin cancer.”
What to look for
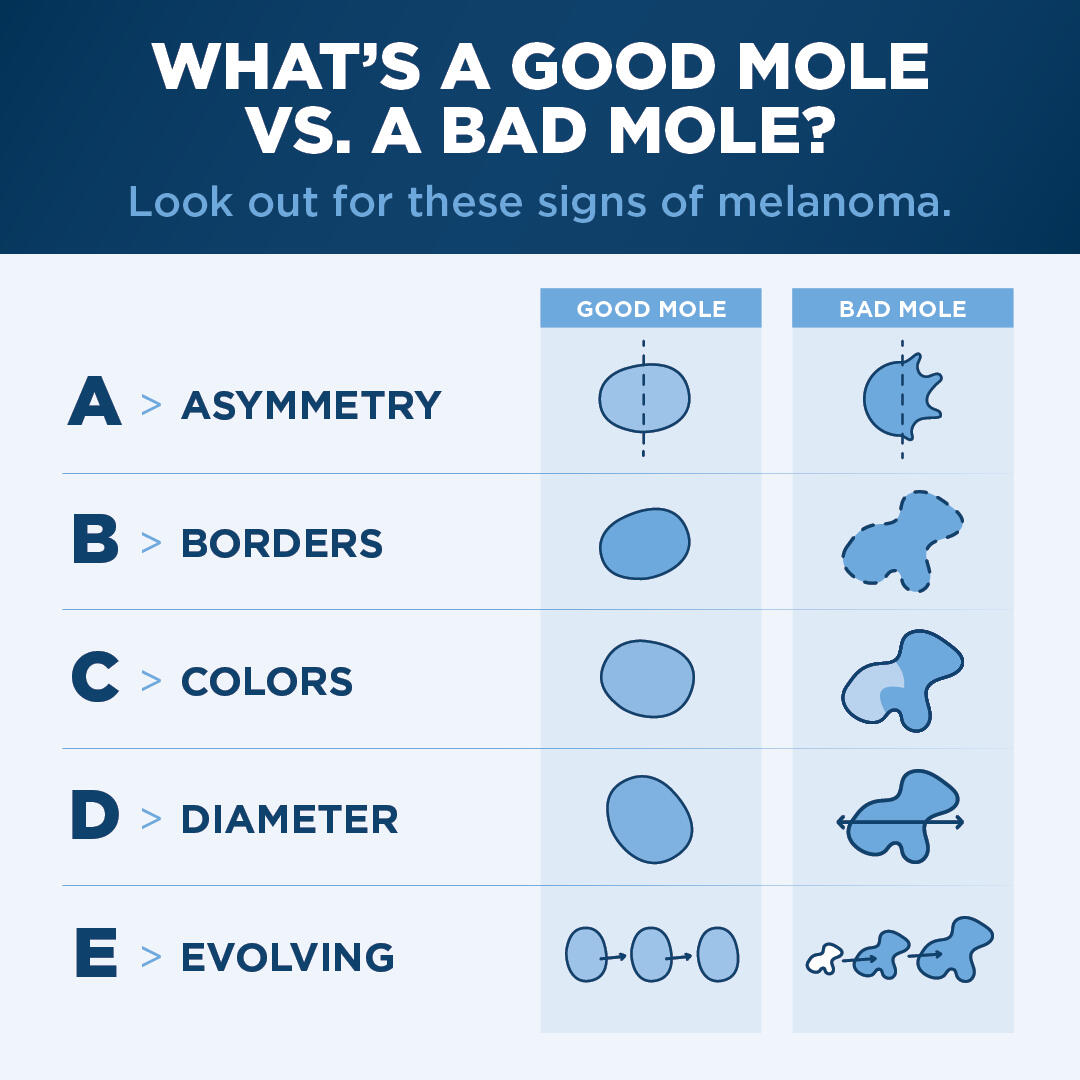
Throughout the year, you should examine your skin head-to-toe, looking for any suspicious lesions. To help you spot possible skin cancer, think ABCDE, Dr. Hoverson suggests:
Enlarge
(Graphic by Sanford Health)
Asymmetry: Draw an imaginary line through the middle of your mole, and the two sides should match, meaning it is symmetrical. When the two halves do not match, that can be a warning sign for melanoma.
Borders: The borders of a melanoma can be irregular, scalloped and sometimes blurred.
Color: Different colors in one mole is considered a bad sign. Different shades of brown, black, and sometimes even red, white, and blue are all concerning.
Diameter: Melanoma is often bigger than regular moles. It is advised to check anything bigger than a pencil eraser that is new or has any other abnormalities.
Evolving: Any mole that grows over time, gets elevated, changes in color, or changes in shape needs to be checked. Also anything that hurts, bleeds or itches.
Shift in priorities
McManus’ melanoma diagnosis made her grow up quickly.
“My carefree years of eating pizza rolls, not getting enough sleep and not caring about exercise were gone,” she says, sipping on a protein shake. “Now I exercise every day, drink lots of water, get enough rest, take vitamins and calcium, and try to eat healthy. My whole life changed.”
She adopted new skin habits, too. Though she’d never spent excessive time in the sun or frequented indoor tanning booths, she took seriously the following steps:
- Consistent use of SPF 50 sunscreen
- Wearing hats
- Choosing shade
- Getting minimal sun exposure between 10 a.m. and 3 p.m.
And for special occasions? She splurges on a professional spray tan.
“It’s the safest option,” McManus says. “So many studies now show a definitive link between tanning (indoor and outdoor) and increased chance of melanoma. It’s not worth it.”
Enlightening others
Her own skin well-protected, McManus works to protect the skin of others, including children. A summer camp counselor, she proudly says, “My kids never get a sunburn.” Her strategy? Just put sunscreen on the checklist of things to do before going out to play.
Staying out of the sun between 10 a.m. and 3 p.m. is ideal, but it is also important to reapply sunscreen regularly, Dr. Hoverson says.
“Every two hours or every time you go into the pool or the lake and get wet, you should reapply,” Dr. Hoverson says. “It’s a big one that can make a difference and a lot of people forget to do it.”
McManus’ own age group isn’t quite as easy, something she’s realized in her job at a bridal shop. She frequently hears young women and their moms mention how much better a formal will look with a tan. She gently offers alternatives like spray tans — or no tan at all.
McManus admits it often falls on deaf ears. “There’s a false sense the bad thing will never happen to them,” she says. “I also think our culture needs to get away from the idea that a tan is healthy and beautiful.”
Sunblock tips
The best sunscreen to use is the one you will apply and reapply, Dr. Hoverson says.
Look for an SPF 30 that blocks about 97% of the UV rays. Anything higher than SPF 30 will give you a slight increase in blocking UV rays, but no sunscreen will block 100%. Don’t skimp when applying. You should apply a shot glass (1 ounce) amount on your body and ½ teaspoon on your face.
Reapplying is key. If you get wet or sweat, make sure you reapply, Dr. Hoverson urges. Creams are better, but powders and sprays – when applied correctly — also do the job.
Spending time in and around the water is always going to warrant special attention.
“If you’re fishing, or just on a boat, you get that reflection off the water,” Dr. Hoverson says. “I tell people they have to be careful with that. Make sure you’re wearing the sunscreen and wearing a wide-brimmed hat. I think a lot of people don’t like the wide-brimmed hats because they blow off in the wind, but they’re the best at blocking out the sun on your face and ears.”
Do you need a skin cancer screening?
Sanford Health recommends a skin cancer screening for people with any of the following:
- A new mole that looks different from the rest
- A personal history of skin cancer
- A family history of multiple skin cancers
- Numerous moles (40+)
- Moles larger than a pencil eraser
- Decades of sun-related skin damage
- A transplant history including immunosuppressive medication
A skin cancer screening is also recommended for anyone who has difficulty doing a thorough check of their own skin — and not just the areas exposed to sun. Melanoma can develop anywhere there are skin cells, including under the fingernails and inside the eyes.
Save your own skin
If something does not look right, tell somebody. Call your primary doctor; visit urgent care; make an appointment with your dermatologist; send a picture. Be proactive. Melanoma is never good, but when found early, it is treatable.
“The important thing is to get it looked at as soon as you can,” Dr. Hoverson says.
And if you’re headed outdoors, grab your sunscreen — then use it.
“Always think two steps ahead,” says McManus. “What you do today will have an impact years from now. It’s easy to skip sunscreen, but it sure isn’t easy going through cancer treatment.”
Learn more
- Spot and prevent skin cancer ahead of time in the sun
- Skin cancer gives patient plenty of Mohs surgery experience
- Keeping you and baby safe and sunburn free
…
Posted In Cancer, Cancer Screenings, Cancer Treatments, Children's, Dermatology, Specialty Care
