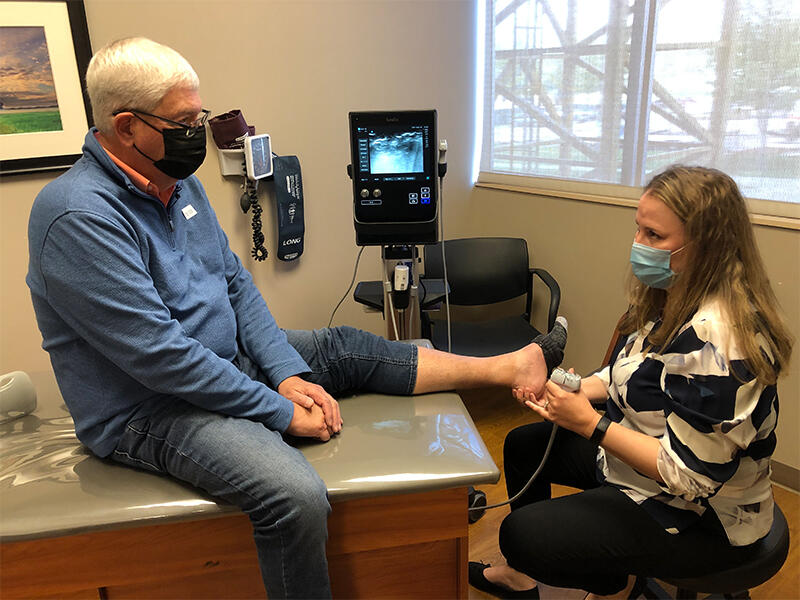
Gary Gillin still might need a new knee.
But before that, he needed treatment on his ankle.
“I may need a knee replacement at some point, but until I get this foot stabilized, I really can’t see rehabbing my knee on a bad foot,” he added.
Lifelong battle
Diagnosed with Haglund’s deformity, a condition where an enlarged heel irritates the Achilles tendon, Gillin has battled chronic knee and ankle pain for years.
“I’ve got an Achilles tendon that’s pretty well irritated, angry and sore,” he said.
Relief for joint pain: Consult with Sanford Orthopedics and Sports Medicine
Gillin said the pain has progressively worsened in the past five to six years, and something needed to be done.
He didn’t want surgery. Not because of the procedure, but because of the recovery.
“The recovery time is anywhere from six to eight months, to a year. So, I wanted to look at something that was nonsurgical, and something that might help the Achilles heal faster,” he said.
PRP treatment an option
That’s when he heard about PRP or platelet-rich plasma treatment from Tiffany Facile, his daughter who works at Sanford Health. PRP is a form of orthobiologic treatment that uses material from a patient’s own body to help heal injuries.
PRP treatment takes plasma from an area of a patient’s body, and is then injected back into the current site of injury.
When asked what was going through his mind when he learned of this treatment, Gillin responded, “anything to reduce the pain.”
“If you’d see me walk on certain days, I’d almost have to club around with like a club foot. It’s that painful. So, I was looking for some kind of relief for the ankle that would be nonsurgical,” he said.
All natural
Gillin said he felt comfortable with the procedure, despite it being a relatively new concept to him. Plus, he said he was truly using his own resources to fight the injury. There wasn’t anything foreign being put into his body.
“It was not a real scary process because it’s already in my body. And, if it can rejuvenate that Achilles and make it less painful, the journey wasn’t too serious.
“The actual procedure itself was great. I mean, there there’s a little discomfort when they numb, but the whole process went very smoothly. I had no pain pills afterwards, I didn’t need anything, and I was very pleased with the way that worked out,” said Gillin.
Post procedure
Right now, Gillin is still in a walking boot, so he still isn’t doing too much walking. Despite that, he said he can already tell a difference in how he feels.
“It’s been about 25 days of pretty much living in the boot. I don’t feel the pain at all while in the boot, which surprises me because before that I could feel the pain just sitting in a chair.
“So, I’m hoping that we’ve got some relief, and it’ll be a long-term thing, so we can kind of move on to normal life again,” he said.
Related: Sanford named top orthopedics hospital in S.D.
He’s most looking forward to simply being more mobile.
And, giving his wife a break from yard duties.
“My wife’s pretty much taken over the lawn mowing jobs and all that kind of stuff. I like to be active, and I would just like to return to that kind of a normal life.”
‘I’d highly recommend it’
Gillin has talked to many specialists about treatment options.
He said none listened to him, or offered him the options the way Sanford Health has.
And, if anyone finds themselves in a similar situation as Gillin, he’d encourage them to seek care at Sanford.
“I’d highly recommend it. I often heard from the orthopedics that I saw, ‘surgery, surgery, surgery.’ But, nobody ever talked to me about what other options are there out there that I should try.
“It made sense to me when I finally made connections with my daughter talking about this process, that it’s something to try before you jump into surgery.”
Learn more
- Achilles rupture: Evolving treatment with Sanford Health
- Sanford tests first umbilical stem cell treatment for COVID-19
- What is regenerative medicine?
…
Posted In Orthopedics, Research, Specialty Care