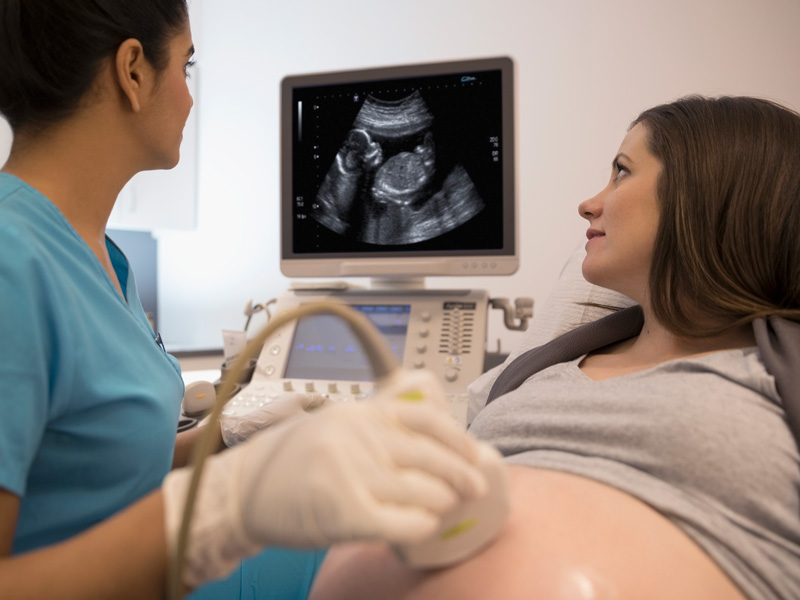
For women currently pregnant in the United States, the risk of dying from a cause related to their pregnancy has more than doubled since some of them were born.
Worldwide, the maternal mortality rate has been trending downward. In the U.S., however, that rate has been rising. According to the Centers for Disease Control and Prevention:
- The U.S. recorded 7.2 deaths per 100,000 live births in 1987
- The rate rose to 17.4 deaths per 100,000 live births in 2018
- Half of those deaths are likely preventable, the CDC estimates
The Joint Commission, which accredits health care organizations, said the U.S. ranks 65th among industrialized countries for maternal mortality.
Meanwhile, Poland, Belarus, Norway and Italy each had just 2 deaths per 100,000 live births in 2017, according to The World Bank.
Sanford Health OB/GYN Ashley Briggs and maternal-fetal medicine physician Peter Van Eerden are working to help save women at risk of dying throughout the Dakotas. Causes of death vary, and disparities persist among races, but the doctors envision ways to keep more women alive.
Dr. Briggs did it herself once in the delivery room several years ago, and that experience contributes to her passion.
She was the doctor on call when a patient experienced a life-threatening condition during delivery. The patient needed an emergency cesarean section and a hysterectomy to save her life and the life of her baby. Dr. Briggs and two other providers cared for the woman during the harrowing delivery.
“Every year, she comes by and thanks us for saving her,” Dr. Briggs said tearfully, “and that her daughter has a mom.”
It frustrates Dr. Briggs to hear stories of women who did not survive pregnancy or childbirth or postpartum complications from something preventable. But she and Dr. Van Eerden hope efforts underway will reduce the number of stories ending in anguish.
Maternal mortality trends
While the vast majority of births result in healthy babies and healthy moms, many circumstances can lead to maternal deaths. Around the world, 94% of maternal deaths happen in low income or lower middle-income countries, according to the World Health Organization. Most of those are considered preventable.
While rates of maternal deaths are high in developing countries, they have been falling significantly, even as U.S. rates have risen.
The CDC says about 700 women die each year in the U.S. because of pregnancy or delivery complications. Thousands more each year survive but face significant short- or long-term health consequences as a result of labor and delivery. This circumstance, called severe maternal morbidity, has been rising as well. In fact, more than 50,000 women were affected by severe maternal morbidity in 2014, the CDC said.
The CDC identified the top causes of pregnancy-related deaths in the U.S.:
- Heart disease and stroke cause most deaths overall.
- Obstetric emergencies, like severe bleeding and amniotic fluid embolism (when amniotic fluid enters a mother’s bloodstream), cause most deaths at delivery.
- Severe bleeding, high blood pressure and infection are most common in the week after delivery.
- Cardiomyopathy (weakened heart muscle) is the leading cause of deaths one week to one year after delivery.
More: Everything you need to know about preeclampsia
Maternal mortality rates vary by race in the U.S., but all are rising. And the disparity among races is widening:
- According to the CDC, the U.S. maternal mortality rate for white women was 10.4 per 100,000 live births during 2005-2007, rising to 13.0 during 2011-2016.
- For Black women, the rate was 34.0 in 2005-2007, rising to 42.4 in 2011-2016.
- For American Indian/Alaska Native women, the rate was 16.9 in 2005-2007, rising to 30.4 in 2011-2016.
- With Asian/Pacific Islander women, the rate was 11.0 in 2005-2007, rising to 14.1 in 2011-2016.
- And with Hispanic women, the rate was 9.6 in 2005-2007, rising to 11.3 in 2011-2016.
Racial disparities
The racial disparities existing in health care in general have recently received attention, raising awareness of the issue. And the maternal mortality aspect of the disparities in particular have concerned Sanford Health OB/GYN Erica Schipper. She serves as the chair for the South Dakota section of the American College of Obstetricians and Gynecologists (ACOG). One recent focus of ACOG has been to try to address the racial differences in maternal mortality.

Preexisting conditions, low socioeconomic status or low education cannot explain away the reason that pregnancy is so much more dangerous for Black women, for example, Dr. Schipper said. A Black woman with advanced education such as a Ph.D., M.D. or law degree is more likely to die as a result of a cause related to her pregnancy than a white woman who completed high school or less.
“We’re slowly learning more and more about historical trauma and the way systemic racism affects people from childhood on,” Dr. Schipper said.
The stress of feeling targeted in society, for example, or that their health concerns won’t be acknowledged can add up over time. Chronic stress can worsen cardiovascular disease, Dr. Schipper said. And avoiding health care can result in poorer health conditions.
“As a physician, I really want to be a part of the solution,” Dr. Schipper said.
Dr. Schipper sees some specific measures that health care providers can take to help support their patients.
For example, they can work to help educate others within and outside of health care. With patients, they can educate about signs and symptoms of pregnancy complications, Dr. Schipper said.
Ensuring patients have access to care and that they feel comfortable seeking that care is key, she said — from prenatal to midwifery and social support to postpartum care.
Care in rural U.S.
Dr. Briggs spent five years serving on the American Indian/Alaska Native Committee for the American College of Obstetricians and Gynecologists. Making site visits throughout the U.S. gave her a firsthand look at the need for improved health care for women in rural locations far from medical centers.
Less than half of rural women live within a 30-minute drive to the nearest hospital offering perinatal services, according to ACOG.
“I really saw how isolated they were, both in distance and in not always having an OB/GYN available to provide maternity care,” Dr. Briggs said.
The providers on hand might include a family practice physician and a general surgeon who could perform C-sections.
“You do still really need to have maternity care … available in those areas and deliveries in those areas,” she added, “because women are already traveling a very far distance.”
Dr. Briggs and other committee members then drafted a publication of standardized recommendations for sites that see few maternity patients to still be able to provide them standard, safe care, ranging from preconception and prenatal care to postpartum care.
Now she serves on a committee closer to home that she helped co-found, along with Dr. Van Eerden, in late 2018 to help reduce maternal mortality in North and South Dakota. Working with people from the March of Dimes and an array of agencies and health care systems from the two states, the North & South Dakota Perinatal Quality Collaborative will select projects to work on to help improve outcomes before and after birth.
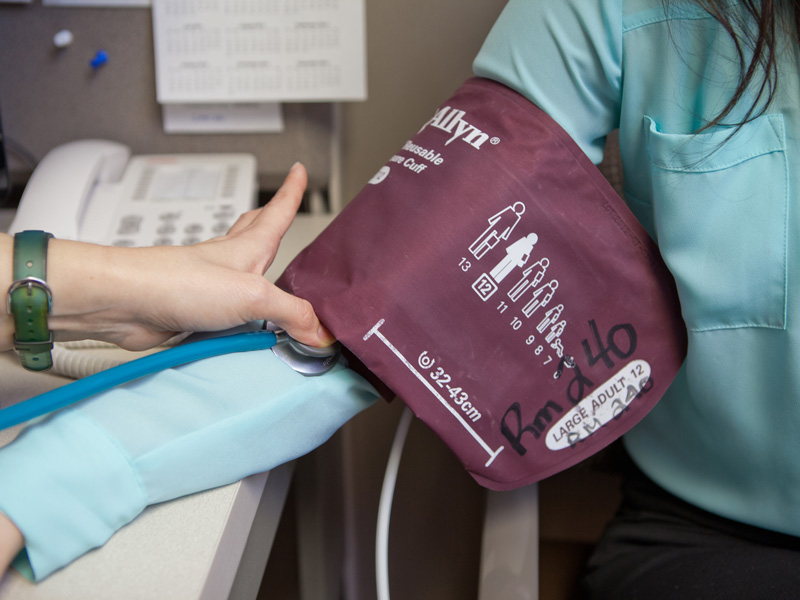
Photo by Sanford Health
High blood pressure project
In November 2019, the Perinatal Quality Collaborative held its first in-person meeting to choose its first initiative, which will last a year. It will focus on making sure that postpartum women who arrive at emergency departments or acute care settings with elevated blood pressure get treated for it within an hour and then get appropriate follow-up care, Dr. Briggs said.
“When these women come in, they need to be treated very differently than if they were not pregnant in the first place or recently pregnant,” Dr. Van Eerden said.
“A normal patient that’s not pregnant can tolerate a much higher blood pressure than a pregnant woman or a postpartum woman,” Dr. Briggs said.
A rare but dangerous condition, preeclampsia — which causes high blood pressure and problems with one or more organs, such as the kidneys — could develop during pregnancy or postpartum. Postpartum preeclampsia can occur immediately after delivery or up to six weeks later. Women might arrive complaining of a headache that won’t go away, blurred vision or flashes of light, or upper abdominal pain on their right side or in the middle of their chest. They might not think to mention they had a baby recently.
To ensure prompt treatment of high blood pressure in women who recently delivered a baby, the collaborative will create webinars to educate providers, ensuring they can recognize symptoms of something they would rarely see, and that blood pressure is being taken uniformly. They’ll have physicians available for support.
They’ll also create a checklist to go through. It will include recommended medications for treating the condition and a phone number for the medical center where the patient is being transported to quickly reach a provider there.
The collaborative will take on projects like this that can improve quality care and patients’ health across facilities, Dr. Briggs said — rural and urban.
Mortality review committees
Dr. Briggs has helped with forming the new Maternal Mortality Review Committee by the Department of Health in South Dakota. Most U.S. states have a committee in place that reviews cases of women who die during or after pregnancy. The goal is to use conclusions from the findings to make suggestions and reduce the mortality rate.
South Dakota saw 10 pregnancy-related deaths from 2010 through 2015, according to the state Department of Health. As the committee starts reviewing cases this year, they’ll look at data and a synopsis collected about each case. They’ll also bring in police or a case manager or a social worker if needed.
“So many different variables could have contributed to a maternal death that we really have to think outside of just the medical part of it,” Dr. Briggs said.
The committee may be able to help address South Dakota’s disparity as well. “There were a lot more Native American women that had passed away compared to the percentage of population that they’re representing,” Dr. Briggs added.
Collecting and analyzing data will be key to focusing on the underlying factors of racial disparities, Dr. Schipper said. Based on the data, she said, “we can start to understand why this is happening, when it’s happening, where it’s happening.”
Dr. Van Eerden, meanwhile, serves on the mortality review committee in North Dakota. That committee would like to have legislation in place to allow it to obtain records and conduct formal reviews of maternal deaths. From there, as in South Dakota’s case, the committee could make recommendations on a state level to improve outcomes.
Standardizing treatments
As a maternal-fetal medicine specialist, Dr. Van Eerden is an OB/GYN with additional education and training to specialize in high-risk pregnancies. He monitors patients in Fargo, North Dakota, and through outreach in rural North Dakota, who may have chronic conditions such as preexisting diabetes, hypertension, obesity or thyroid disease.

In addition, he sees patients with pregnancy complications such as multiples, growth restriction, fetal genetic conditions or anomalies, or risk of preterm birth. He also performs high-level ultrasounds and takes care of pregnant patients admitted to the hospital with complications.
But that’s not all he does.
“I see my job as not only taking care of the patients primarily, but also helping providers who take care of pregnant women stay up to date with current standards and guidelines of our national organizations,” he said.
He works to help reduce not only maternal mortality but also severe maternal morbidity — sickness that pregnancy causes or makes worse for women who have given birth. Dr. Van Eerden has been helping to implement standardized patient safety “bundles,” or toolkits, at his hospital, Sanford Medical Center Fargo, through his leadership on the Sanford Fargo Quality and Safety Committee.
California’s Maternal Quality Care Collaborative has contributed to a dramatic drop in maternal deaths in that state since it started developing and implementing bundles. Each bundle takes a different issue, Dr. Van Eerden said, “and gives you background and literature and evidence-based guidelines as to exactly what to do and who to take care of and how to take care of them.”
The Fargo committee is working hard on ensuring that the recommended guidelines are in place for obstetric hemorrhage and hypertension, implementing staff education along with simulations and drills. Additionally, the focus is on venous thromboembolism, which involves determining who should be taking blood thinners during pregnancy and postpartum to prevent blood clots.
More efforts at Sanford Health
With an eye on decreasing the U.S. maternal mortality rate, the Joint Commission set two new standards for hospitals that go into effect July 1 and include several specific elements. One standard addresses postpartum hemorrhage; the other addresses severe hypertension/preeclampsia.
For example, one aspect of the postpartum hemorrhage standard involves placing a specific drape, with a clear plastic bag, under the mom to collect and measure the amount of blood she loses immediately after delivery. This quickly, visually indicates when blood loss is greater than it should be.
One part of the hypertension standard involves treating high blood pressure within an hour. To help make the “danger zone” of blood pressure for a pregnant woman more obvious, Dr. Briggs and others at Sanford USD Medical Center in Sioux Falls worked with the technology staff to highlight abnormal pressure for pregnant women as a red number. That immediately signals that it’s time to involve a nurse, who can solicit orders for treatment from the provider.
“That changed it for the whole Sanford system,” Dr. Briggs said.
Other measures Sanford Health has taken to help address maternal mortality, Dr. Briggs added, include ensuring open communication between referring providers in rural areas and specialists at the regional medical centers. Standardized care among all facilities has helped. And a rural OB/GYN has developed a mobile program aboard a truck to provide drills and simulations at rural hospitals that offer labor and delivery services.
“Sometimes, it’s hard for each smaller place to develop all of this,” Dr. Briggs said. But this way, they can practice for rare emergency situations and be better prepared to save a life.
Family planning to improve safety
Another key part of preventing maternal deaths, Dr. Briggs said, is making sure the pregnancies are planned — and prepared for.
What she sees in her work with patients, she said, falls in line with the South Dakota Department of Health’s conclusion that a rise in chronic health conditions is causing part of the rise in the maternal mortality rate. Increased reporting is seen as another major factor.
“I’m seeing more hypertension, diabetes, chronic heart disease in these pregnant women,” Dr. Briggs said. “It’s putting them at greater risk for these complications.”
Nearly half of all pregnancies in the U.S. are unintended, according to the CDC. So Dr. Briggs believes keeping women safe and healthy starts before pregnancy, with planning.
Playing a role in planning is, she said, “effective contraception so that women can have their children when they want them.”
Pregnancy spacing helps women manage chronic medical conditions in between pregnancies as well, she said.
Dr. Briggs highly recommends that women who are thinking about becoming pregnant make an appointment for a preconception visit so they can discuss managing any medical issues of concern beforehand.
It’s also important, she added, for women to call their doctor’s office as soon as they have a positive pregnancy test. At that point, they can review medications the mom is currently taking, review medical issues, take a health history and make sure they’re not feeling extreme nausea. They can also do an early ultrasound to try to accurately date the pregnancy.
Screening to help with planning
To help encourage healthy pregnancies, Dr. Briggs is working on implementing a screening program at Sanford Health. Called One Key Question and embraced by the March of Dimes, the program prompts the provider to ask women of reproductive age, while they are in for an appointment, whether they would like to become pregnant in the next year.
If they answer yes, Dr. Briggs said, they would be offered a preconception visit to go through their health history and any medical concerns. If they answer no, the discussion would turn to effective contraception methods.
Whether it’s working with patients at her clinic or working with colleagues on committees, Dr. Briggs has committed herself to helping women have the healthiest, safest pregnancies they can.
She feels fortunate to have been part of saving a patient’s life during delivery, especially when she attends national meetings where presentations refer to patients who didn’t survive because of conditions that went unrecognized.
“One dad watched his wife die in front of him. … He knew something was wrong, and no one would help him. And she bled to death,” Dr. Briggs said.
Lowering mortality rates means saving the life of a woman. It preserves pregnancy and childbirth as a family’s time of joy — not a time of sorrow.
Learn more
- Sen. Tina Smith convenes maternal health roundtable
- Postpartum bleeding follows festive, ‘picture-perfect’ birth
- 8 warning signs during pregnancy
…
Posted In Healthy Living, Here for all. Here for good., Pregnancy, Rural Health, Specialty Care, Thought Leadership, Women's